Why treatment in Wilson’s Disease is never just about symptoms
When Wilson’s Disease reaches the point where treatment is being discussed, most patients have already gone through a phase of uncertainty where symptoms didn’t quite connect, reports didn’t give a clear answer, and the condition itself didn’t behave in a predictable way. By the time a diagnosis is confirmed, there is usually already some degree of copper accumulation that the body has been dealing with quietly for a long time, because this is not a condition where things change overnight but one where the imbalance builds slowly until the liver can no longer contain it.
What makes Wilson’s Disease different from many other conditions is that the problem is not something new entering the body, but something normal that the body has stopped handling properly, and that changes the entire approach to treatment because the focus is not on blocking or suppressing, but on removing what has already built up. Copper continues to enter the system through diet just as it always has, but the liver is no longer able to move it out through bile the way it should, and once storage capacity is exceeded, that copper begins circulating in a form that is far more reactive and damaging to tissues.
This is the stage where treatment becomes necessary, not because symptoms are severe in every case, but because the process itself does not slow down on its own.
Where trientine actually steps in
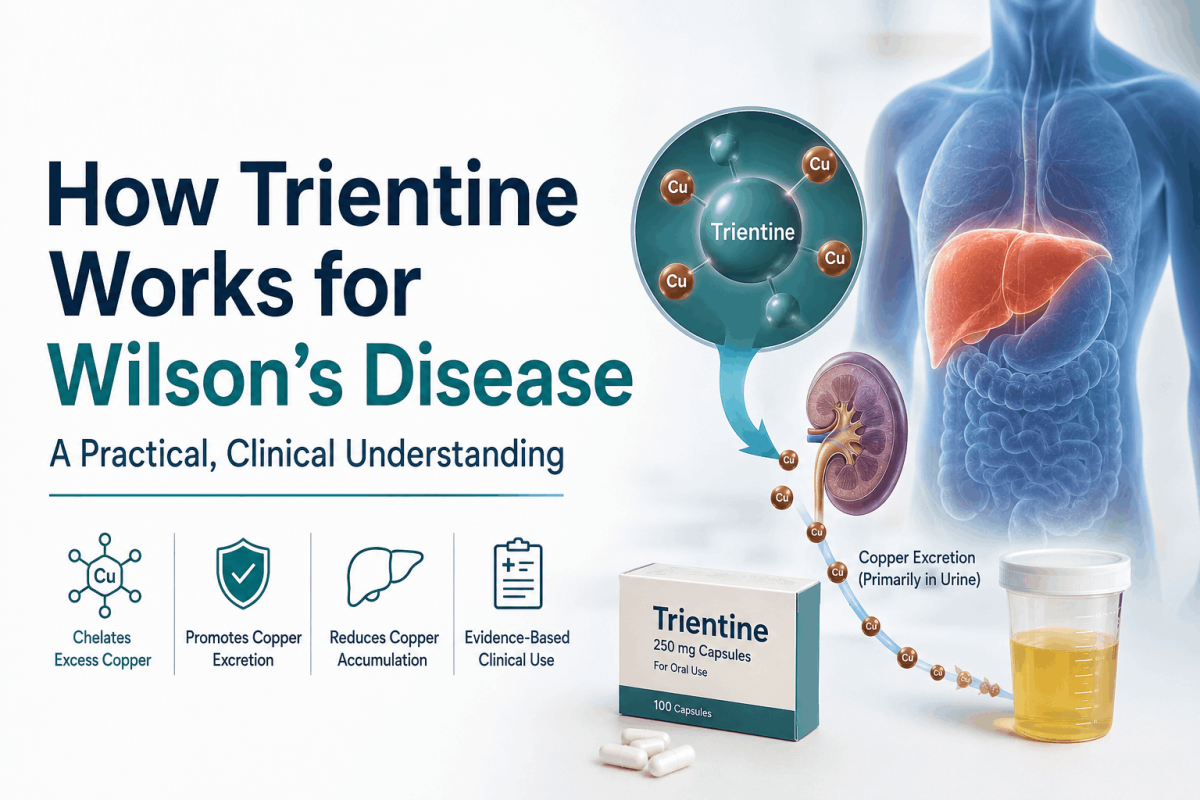
Trientine does not interfere with copper entering the body, and it does not attempt to repair the underlying genetic issue, which is important to understand early on because expectations around treatment often become clearer once this is understood properly. What it does instead is much more direct and, in a way, more practical — it binds to copper that is already present in excess and allows the body to remove it through a route that is still functioning.
In Wilson’s Disease, the usual route of copper elimination through bile is compromised, but the kidneys are still capable of filtering substances from the bloodstream, and trientine uses that pathway. Once it binds to free copper, the complex that forms is stable enough to circulate safely and small enough to be filtered and excreted in urine, which creates an alternate exit route for something the body is otherwise unable to clear.
In clinical practice, this is what makes trientine effective, because it does not depend on a system that is already failing, and instead works around it.
What really happens after starting trientine
The beginning of treatment is often quieter than people expect, and this is where many patients start questioning whether the medicine is doing anything at all, because there is no immediate shift in how the body feels. There is no sudden drop in fatigue, no immediate improvement in appetite, and no visible sign that copper is being reduced.
But internally, the process has already started.
Copper that is circulating in its free form begins to get bound, and as that pool starts to reduce, copper that has been loosely held in tissues begins to move back into circulation where it can also be cleared. This is not something that happens all at once, and it is not something that can be rushed, because the body has been accumulating copper over a long period of time and needs to offload it gradually to avoid further imbalance.
This is also why urinary copper levels increase after starting treatment, which often confuses patients when they first see the reports, because it looks like copper levels are going up when in reality the body is finally getting rid of it.
Over time, as this process continues, the overall copper burden starts to come down, and that is when changes begin to reflect in liver function tests and, eventually, in how the patient feels. But that gap between starting treatment and feeling improvement is something that needs to be understood clearly, otherwise it becomes easy to assume that nothing is happening.
Why trientine often becomes the more practical long-term option
In theory, more than one chelating agent can be used in Wilson’s Disease, but in real-world practice, the choice of drug is often shaped by how well a patient is able to continue it over time rather than how quickly it works in the beginning. Penicillamine has been used for years and remains effective, but it is not uncommon to see patients struggle with side effects that make it difficult to maintain consistency, and in a condition like this, inconsistency is where problems begin.
Trientine Hydrochloride 250 mg Capsules tends to be easier for many patients to stay on, not because it is fundamentally different in what it achieves, but because it is often better tolerated over longer durations. That difference may seem small when looked at from a purely pharmacological perspective, but in practice it becomes one of the most important factors in determining whether treatment continues uninterrupted.
And in Wilson’s Disease, continuity is not optional.
Once copper levels begin to come down, they have to be kept down, because the body has not regained the ability to manage copper independently, and stopping treatment does not pause the disease, it simply allows the same process to start building again in the background.
The part of treatment that usually gets underestimated
There is a phase during treatment where patients start feeling relatively stable, and this is where the perception of the disease begins to shift, because symptoms are no longer as prominent and daily life starts returning to a familiar pattern. It is also the point where medication can begin to feel less urgent, especially when nothing seems to be going wrong.
But this is exactly the stage where the role of trientine becomes most important, because the absence of symptoms does not mean the underlying issue has been resolved, and copper metabolism has not corrected itself in the background. Copper continues to enter the body, and without chelation, it will begin accumulating again in the same way it did before.
This is why treatment in Wilson’s Disease does not follow the pattern of “take until better and then stop,” and why doctors emphasize adherence even when everything appears stable.
Access in India and why it has mattered more than expected
For a long time, one of the less discussed challenges in managing Wilson’s Disease in India has been access to the right medication, particularly trientine, which despite being a well-established treatment has not always been easy to obtain consistently. Patients often found themselves depending on limited suppliers or dealing with delays that interrupted therapy, and those interruptions, even when short, were enough to affect long-term control.
This is where the availability of Triokris, introduced by Ikris Pharma Network, has started making a practical difference, because it provides a more dependable option within the country, reducing the uncertainty that patients previously had to deal with when trying to continue treatment. For clinicians as well, this changes how confidently they can plan long-term therapy, knowing that the medication is more consistently accessible rather than something that patients may struggle to find after prescription.
In a condition where the treatment itself is already long-term, removing uncertainty around availability is not a small improvement, it is part of making the treatment actually work in real life.
What Taking Trientine Actually Looks Like in Real Life
Once trientine becomes part of treatment, the conversation slowly shifts from “what the drug does” to “how it fits into daily life,” and this is where the difference between theory and practice becomes very clear, because managing Wilson’s Disease is not just about prescribing the right medicine, but about making sure that it can be taken consistently in a way that actually works for the patient over months and years.
Trientine is not taken casually or interchangeably with other medications, because its absorption and effectiveness depend on how it is spaced in relation to food and other substances, particularly minerals like iron and zinc that can interfere with its binding capacity, which is why it is usually advised to be taken on an empty stomach, often one hour before meals or two hours after, even though in real-life settings this timing sometimes needs to be adjusted depending on the patient’s routine and tolerance.
For many patients, this becomes one of the first adjustments they have to make, because unlike short-term medications that are taken for a fixed duration, this is something that needs to fit into everyday life without being skipped, and small inconsistencies, especially in the early phase, can affect how effectively copper levels begin to come down. Over time, most patients find a rhythm that works for them, but that initial phase requires attention, not just to dosage, but to how the medication is actually being taken.
The dosage itself is not fixed in a one-size-fits-all way, because it depends on factors like body weight, stage of disease, and how the patient is responding to treatment, and it is usually adjusted based on urinary copper excretion and clinical markers rather than symptoms alone, which means follow-ups are not just routine check-ins but an essential part of how treatment is shaped over time.
From the outside, monitoring can sometimes feel repetitive, especially when multiple tests are being done over time, but each of them has a very specific purpose, and understanding that makes the process easier to follow rather than feeling like an endless cycle of reports.
One of the most important markers is 24-hour urinary copper excretion, which helps indicate how much copper is being removed from the body, and in the early phase of treatment, this value is expected to be higher as the body starts clearing accumulated copper, gradually stabilizing as levels come under control. This is often paired with liver function tests, not because they change dramatically overnight, but because they show whether the liver is stabilizing or continuing to remain under stress.
In some cases, especially where neurological symptoms are involved, clinical observation becomes just as important as lab values, because improvements in coordination, speech, or tremors do not always follow the same timeline as biochemical changes, and interpreting progress requires looking at both together rather than expecting them to align immediately.
There is also a need to ensure that copper levels do not drop excessively, because while the primary concern is accumulation, overcorrection can affect essential physiological processes, which is why treatment is always guided rather than left static, and adjustments are made based on how the body is responding rather than following a rigid plan.
Side Effects, Not as a List, but as Something to Recognize Early
Trientine is generally better tolerated compared to older chelating agents, but that does not mean it is completely free of side effects, and the way these are approached in practice is less about memorizing a list and more about recognizing patterns early before they become significant.
Some patients may experience mild gastrointestinal discomfort when starting treatment, which usually settles as the body adjusts, while others may notice changes that need closer evaluation, such as unexplained fatigue that feels different from baseline, or symptoms that do not align with the expected course of recovery. In rare cases, issues related to iron metabolism can arise, because trientine can bind not only copper but also iron to some extent, which is why spacing between supplements and medication becomes important.
What matters most is not reacting to every small change, but not ignoring persistent ones either, because early communication with the treating physician allows adjustments to be made without interrupting treatment altogether, which is always the goal.
In day-to-day life, patients are rarely taking just one medication, and this is where interactions become relevant, not in a theoretical sense, but in how they affect the actual effectiveness of treatment.
Mineral supplements, particularly iron and zinc, can interfere with trientine if taken too close together, reducing its ability to bind copper effectively, which is why spacing becomes necessary rather than optional. Even antacids and certain over-the-counter medications can affect absorption, which is something that is often overlooked unless specifically discussed.
This does not mean patients need to avoid everything, but it does mean that timing matters, and once that is understood, it becomes part of routine rather than a complication.
With time, something shifts in how trientine treatment is experienced, because the initial phase, which involves adjustment and uncertainty, gradually settles into a more predictable pattern where medication becomes part of the daily routine rather than something that constantly needs attention.
What does not change, however, is the need for consistency.
Even when reports stabilize and symptoms are controlled, the underlying metabolic issue remains, and stopping treatment, even briefly, allows copper to begin accumulating again in the same way it did before, often without immediate warning signs. This is why long-term use is not described in terms of duration, but in terms of continuity, because the benefit of treatment depends entirely on it being maintained.
For many patients, this realization does not come immediately, but once it does, the approach to treatment becomes more stable, because it is no longer driven by how one feels on a given day, but by an understanding of what is happening in the background.
In practical terms, all of this depends on one thing that often gets overlooked in clinical discussions—availability.
For years, trientine has been known as an effective treatment, but in India, access has not always been straightforward, which has affected how consistently patients are able to stay on therapy, regardless of how well the drug works on paper. Interruptions due to supply issues have been a real concern, not just an inconvenience, because they directly impact how well copper levels are controlled over time.
With Triokris, made available by Ikris Pharma Network, this situation has started to change in a way that is noticeable at a patient level, because having a more reliable source within the country reduces the uncertainty around continuing treatment, and that stability allows both patients and doctors to focus on managing the condition rather than managing access to the medication.
It does not change how trientine works, but it changes how consistently it can be used, and in Wilson’s Disease, that difference is significant.
Trientine treatment is often explained in terms of chemistry and mechanism, but its real value becomes clearer when seen over time, because it is not just removing copper, it is preventing the same cycle of accumulation from repeating itself.
The effectiveness of the drug does not depend on how quickly it works, but on how steadily it is used, and once that rhythm is established, the condition becomes something that can be managed rather than something that continues to progress.
And in that sense, trientine is not just a treatment that is started at diagnosis, but one that continues quietly in the background, doing exactly what the body is no longer able to do on its own.